Note - This is an a online e log book to discuss our patient's de-identified health data shared after taking his / her / guardians signed informed consent. Here we discuss our individual patients problems through series of inputs from available global online community of experts with an aim to solve those patients clinical problem with collective current best evident based input.
This E blog also reflects my patient centred online learning portfolio and your valuable inputs on the comment box is welcome.
I have been given this case to solve in an attempt to understand the topic of " patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations and come up with diagnosis and treatment.
SHORT CASE
A 28 year old male came to the OPD with the chief complaint of blood in stools since 1.5 years and shortness of breath on exertion since 1 year.
HISTORY OF PRESENTING ILLNESS-
The patient was apparently asymptomatic 18 months back then he noticed blood in his stools, about few drops of red blood, once every 1 to 2 months,which is not associated with any pain during defecation.
There is no h/o abdominal pain, constipation, hemetemesis.
No mass per rectum.
He has been experiencing difficulty in breathing on exertion (NYHA grade 2) since 12 months.
He has h/o palpitations and tremors since 6 months.
He developed fever 10 days back which is of low grade, continuous and associated with chills. He was prescribed paracetamol by the local rmp but the fever did not subside. He was then sent to the local hospital in Miryalaguda where he was found to have decreased hemoglobin.
Hb-2.1%
RBC-1.5 million /mm3
Platelets- 1lakh
He was then referred to our hospital for gastroenterologist.
Here he was transfused blood owing which his Hb increased as follows -
He recieved another unit of blood (PRBC) on the afternoon of 21-8-22.
PAST HISTORY -
He is suffering from poliomyelitis since the age of 5 yrs due to which his left lower limb is paralysed and wasted.
He is not a k/c/o HTN, DM, TB, asthma, CAD, CVA and epilepsy
TREATMENT HISTORY-
He had undergone a surgery in his left thigh for releasing the contracture due to polio.
PERSONAL HISTORY-
He is a post graduate student whose daily activity includes studying at home.
Appetite - low ( from childhood)
Diet - mixed
Bowel & bladder habits - regular
Sleep - adequate
Addictions - none
FAMILY HISTORY-
No significant family history
GENERAL PHYSICAL EXAMINATION-
The patient is conscious, coherent and cooperative and well oriented to time, place and person.
He is lean built.
Pallor - present
Icterus - absent
Cyanosis - absent
Clubbing - absent
Generalised lymphadenopathy - absent
B/l pedal edema - absent
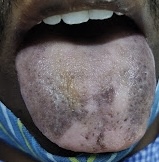
Hyperpigmentation (tongue, knuckles)
Video links for -
VITALS -
Temp - 98 degree F
PR - 89bpm
RR- 20cpm
BP - 110/90mmof hg
Spo2 - 98% at room air
SYSTEMIC EXAMINATION-
CVS - S1 , S2 heard , no murmurs
CNS - Higher mental status- N
Cranial nerves- intact
Motor -
Tone- normal (left lower limb- hypotonic)
Power- normal (left lower limb-no power)
Reflex- B S T K A P
Rt- ++ ++ ++ + + flexion
Lt- ++ ++ ++ - - -
Cerebellar functions- N
Gait- walks by supporting his left lower limb with left hand
RESPIRATORY SYSTEM - BAE- present, trachea - central, NVBS heard
ABDOMEN - soft, non tender, mild splenomegaly present
PROVISIONAL DIAGNOSIS- Severe anemia secondary to bleeding PR(?hookworm infestation)
Autoimmune polyglandular syndrome(? Thyroiditis, Addison's dis, vit B12 def anemia)
LAB INVESTIGATIONS -
On 18-8-22
Hb: 2.5mg/dl
Total count: 3000
RBC: 1.74
PCV: 9.4
MCV: 53.7
MCH: 14.4
MCHC: 26.9
RDW: 20
On 19-8-22
Hb: 3.5mg/dl
Total count: 4500
RBC: 1.9
PCV: 11.1
MCV: 58.6
MCH: 18.3
MCHC: 31.2
RDW: 40.3
On 20-8-22
Hb: 4.8mg/dl
Total count: 7600
RBC: 2.54
PCV: 15.2
MCV: 59.8
MCH: 18.8
MCHC: 31.5
RDW: 33.6
Serum iron - 92mg/dl
LFT -
Total bilirubin: 2.62 mg/dl
Direct bilirubin: 0.46 mg/dl
SGOT: 24
SGPT: 10
ALP: 151
Total protein: 6.1g/dl
Serum creatinine: 2.1mg/dl
Blood urea: 77mg/dl
CUE - normal
Serum electrolytes-
Sodium: 138meq/l
Potassium: 3.4meq/l
Chloride: 104meq/l
ECG -
Mild splenomegaly
PROCTOSCOPY - no mass seen,no haemorrhoids
PR examination - no skin tags, 2 fissures present at 5'o clock position
no masses felt
anal tone - normal
stool stained fingers
TREATMENT PLAN -
PRBC transfusion
Inj. LASIX 20mg I.V sos
Inj. VITLOFOL OD
Tab. BANDYPLUS
Adviced -
High fibre diet
ANOBLISS ointment
Syrup CREMAFFIN
SITS bath/ with betadine TID






Comments
Post a Comment